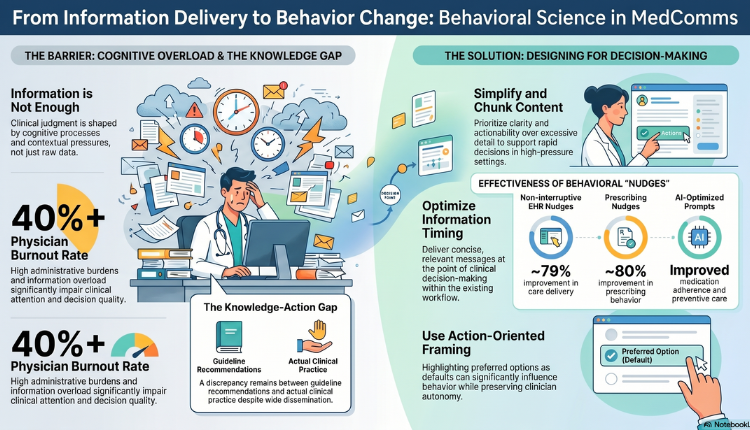
Healthcare today operates in an information-rich environment. Clinical guidelines, peer-reviewed research, and real-world evidence are widely accessible. Yet, a persistent gap remains between what clinicians know and what they do, with a consistent discrepancy between guideline recommendations and actual clinical practice. Evidence-based recommendations are not always consistently implemented in practice, despite being widely disseminated through medical communication channels.
This gap between information and action highlights a key limitation of traditional medical communications (MedComms): the assumption that providing accurate and comprehensive medical content is sufficient to drive behavior change. In reality, clinical judgement is shaped not only by knowledge, but also by cognitive processes, time constraints, and contextual pressures.
This is where behavioral science offers a way to bridge this divide by focusing on how clinicians process clinical evidence and make decisions in routine clinical practice.
The Real Problem: Cognitive Overload in Clinical Practice
Clinicians often operate under time pressure, which can influence clinical decision-making and information processing. The growing reliance on electronic health records (EHRs), clinical dashboards, and data-rich reports has further intensified these demands, often exceeding cognitive capacity.
In such an environments, the ability to interpret and apply clinical evidence is constrained. Information overload has been linked to reduced attention, impaired clinical judgement, and an increased risk of errors in clinical settings. More information does not necessarily translate into better decisions.
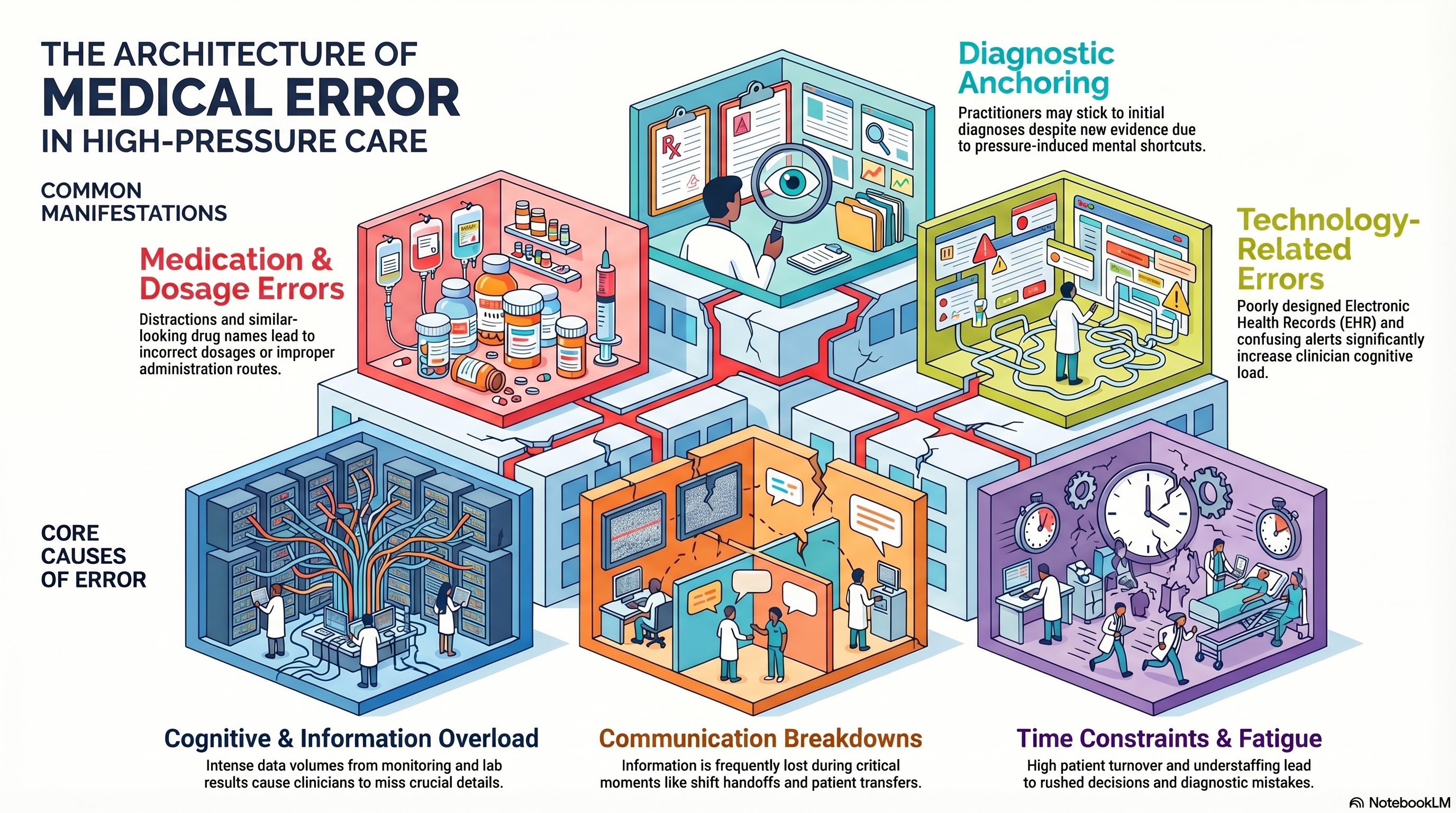
(Disclosure: The above image is generated using Notebook LM for illustrative purpose.)
These challenges are further reflected in rising burnout levels. Recent survey data indicate that more than two in five primary care physicians report burnout, largely driven by administrative burdens.
To address these constraints, communication must aim to reduce cognitive effort. The goal is not to simplify the science itself, but to present it in a way that aligns with how clinicians process clinical context under healthcare delivery settings.
Behavioral Science: Understanding Real-World Decision-Making
Behavioral science examines how people make decisions in practice, acknowledging that choices are shaped by context, constraints, and cognitive biases. It challenges the assumption that individuals always act rationally when presented with complete information.
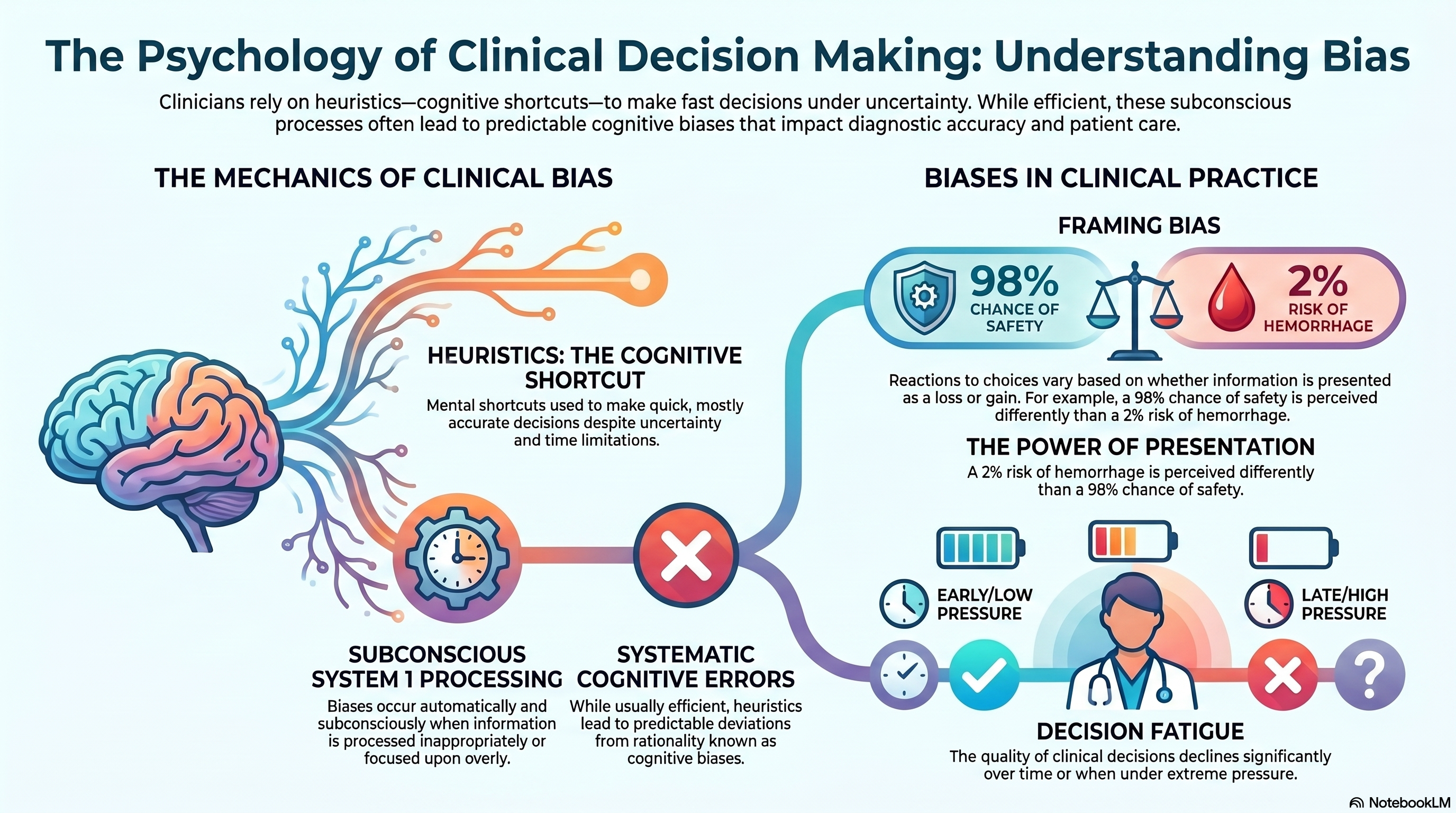
(Disclosure: The above image is generated using Notebook LM for illustrative purpose.)
Several concepts are particularly relevant to medical communications (MedComms).
- explain why clinicians may default to familiar practices or habitual practices.
- highlights how the presentation of information can influence interpretation.
- Decision fatigue shows how the quality of decisions may decline over time or under pressure.
Applying these insights shifts the role of MedComms. Instead of focusing solely on information delivery, communication can be designed to actively support clinical reasoning. In this sense, MedComms can function as a behavioral intervention, helping clinicians navigate complexity more effectively.
The Missed Opportunity: Nudges in Healthcare vs MedComms
Nudges are subtle changes in the design of environments or the framing of information that influence behavior without restricting choice. Within healthcare systems, these principles are already widely applied in clinical workflows to improve patient outcomes and transform healthcare delivery.
Behavioral nudges embedded in EHR systems influence clinical decision-making across care settings. A cluster randomized trial showed that clinician- and patient-facing nudges increased statin prescribing and improved adherence to cardiovascular prevention guidelines by altering decision architecture. Similarly, an EHR-linked intervention improved antihypertensive medication adherence in cardiometabolic disease, highlighting the role of real-time prompts in chronic disease management.
However, such principles are not consistently applied in medical communications. Content often remains static, text-heavy, and disconnected from point-of-care contexts. This represents a missed opportunity. If small design changes can influence clinical behavior, the same approach can be applied to MedComms—using structure, format, and timing to better support clinician decision processes without altering the underlying evidence.
Applying Behavioral Science in Medical Communications
Translating behavioral insights into practice requires intentional design choices. Several strategies can significantly enhance the effectiveness of medical communications:
Simplify the Decision
Clinicians must make rapid decisions in high-pressure settings. Communication should prioritize clarity and actionability over excessive detail. Clear summaries, key takeaways, and explicit recommendations reduce ambiguity and support faster decision-making. Research on non-interruptive EHR nudges shows they reduce alert fatigue and improve care delivery (~79%) by guiding decisions through better visibility and optimized defaults.
Guide Attention Through Visual Hierarchy
Information structure plays a key role in how effectively it is understood and acted upon. Using headings, bullet points, and visual hierarchy directs attention to key messages. Chunking information into manageable sections also improves comprehension and recall. Evidence on visual hierarchy shows that emphasizing key information through layout, positioning, and visual prominence helps clinicians process information more quickly and accurately.
Reinforce Key Messages
Repetition and consistency support behavior change. Research shows that brief, theory-based messages can effectively influence health behaviors and intentions by reinforcing key cues and improving engagement over time.
Deliver Information at the Right Time
Information is most effective when delivered at the point of clinical decision-making within the workflow. Poorly timed or excessive alerts contribute to alert fatigue, making concise, relevant, and well-timed communication more impactful than interruptive or overloaded messages.
Use Action-Oriented Framing
Framing recommendations in a clear and directive manner can significantly influence behavior. Highlighting preferred options or recommended actions acts as a nudge while preserving clinician autonomy. Evidence from prescribing interventions shows that most nudges (~80%) improve prescribing behavior, with the strongest impact seen when recommended options were set as defaults.
Together, these strategies help transform medical communications into tools that actively support clinical reasoning rather than passively delivering information.
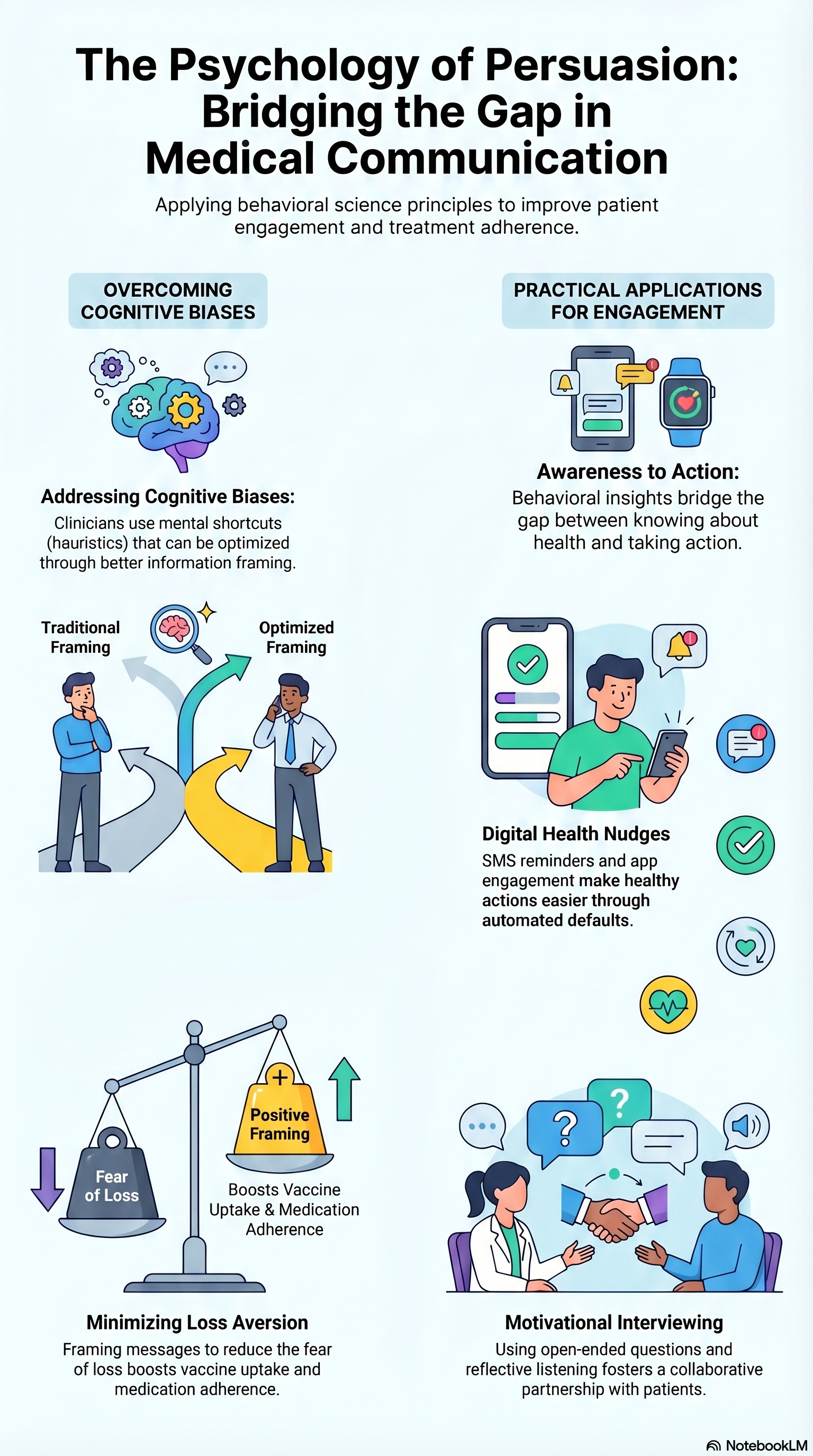
(Disclosure: The above image is generated using Notebook LM for illustrative purpose.)
The Future of MedComms: Behavioral Intelligence Meets AI
The future of MedComms lies at the intersection of behavioral science, digital technology, and artificial intelligence (AI). AI enables personalized, adaptive communication by tailoring content to user behavior, preferences, and engagement patterns. When combined with behavioral science, it operationalizes nudging, timing, framing, and reinforcement to improve adherence, comprehension, and clinical decision-making.
This convergence is already emerging across multiple applications.
- Generative AI can design behaviorally optimized SMS interventions that deliver “just-in-time” health prompts to support preventive care, follow-ups and timely patient action.
- AI chatbots offer a more personalized, engaging, and on-demand user experience that support health behaviors, particularly in chronic disease management such as hypertension care.
- In clinical settings, ambient AI documentation reduces cognitive and administrative burden by converting patient–clinician conversations into structured records, freeing up time for more meaningful communication.
- Voice-based conversational systems are expanding access to care, particularly for elderly and low-literacy populations, by delivering reminders and guidance in natural, accessible language formats.
Despite this progress, implementation science in this area remains underdeveloped. There is a need for more research on clinician trust, patient engagement, and organizational readiness to fully realize the potential of AI-enabled behavioral interventions.
Ultimately, MedComms is evolving from static content creation to dynamic decision support where behavioral science will play a central role in this transformation.
Conclusion: Designing for Decisions, Not Just Delivery
The real opportunity for medical communications lies in moving from content creation to decision design. This means prioritizing clarity over completeness, timing over volume, and action over passive awareness. Integrating behavioral thinking into core functions such as medical writing, medical education, and evidence dissemination (including health economics and outcomes research [HEOR] and real-world evidence [RWE]) can help ensure that communication is built around how clinicians actually engage with clinical content.
Looking ahead, the focus should be on creating communication that fits naturally within clinical workflows and supports faster, more confident decisions. The shift is subtle but significant: from asking what information to share to how that information will be used in practice. That is where meaningful impact begins.